 A patient receiving devastating news cannot reach for the hand of a family member for confidence and assurance, is therefore left with the hand of their healthcare provider for support instead. Through participation in video conferencing sessions between patients and families, healthcare providers cannot help but feel and absorb the added emotions in the room. With the lack of visitor presence in the hospital setting, nurses, physicians, and other allied healthcare staff strive to balance an increase in usual duties while simultaneously providing emotional support and physical presence to end-of-life patients. Regrettably, due to the restrictions to in-hospital visitors, the comfort of human physical contact and presence has been replaced by a more distant interaction of video conferencing. For patients suffering from a cognitive impairment, a video conference may create more confusion and anxiety. Virtual communication has replaced face-to-face in-hospital visits and phone calls and has provided comfort to some, but not to all patients. Both the social work and spiritual care departments have been integral at assisting patients with access to videoconferencing, especially those who are not already virtually connecting. Consequently, our institution introduced video conferencing methods to patients and their families and friends to promote and enhance communication. Both options bring new stressors to families highlighting the concern of more complicated grief after death.Īnother important challenge faced by practitioners due to visitor restrictions, as a result of COVID-19, is the negative impact on communication between patient and family and between patient, family, and heathcare providers. Families must decide between having their loved one at home and being in the presence of relatives, or have end-of-life care managed in an institution, knowing that family time would now be greatly diminished and restricted due to the COVID-19 visitor policies. In addition to prior difficult decisions patients and families often face at end of life, they must now make decisions regarding place of care with new implications. Due to these new restrictions on visitors, patients and families have been faced with additional difficult end-of-life care decisions. While these policies are wisely enforced for the greater good to prevent the spread of the coronavirus, the impact on patients and their families/friends can be devastating. The aim of the restricted visitor policies is stringent infection control by limiting the incidence of asymptomatic carriers into the hospital who could be carrying the virus. Therefore, the final moments families are spending with dying patients are hallmarked by limited communication and, quite possibly, unsettling physical appearances. Patients may also be demonstrating some of the more physically overt symptoms of the dying process, such as agonal breathing, upper airway secretions or terminal delirium, which can be distressing for families to witness. The allowance of visitors in the last 48 hours is especially challenging as, at that time, many patients are unresponsive, and meaningful communication with family is limited. Additionally, those dying patients who do not have coronavirus are limited to a maximum of only two visitors in their last 48 hours of life, with only one visitor allowed at a time. Hospitalized patients with COVID-19 are not allowed visitors, even when dying. Unfortunately, this practice is no longer permissible during these unprecedented times. 
Often times a support person might accompany a patient throughout the day or night. Prior to the global pandemic, a dying patient was able to have countless visitors with loved ones gathered at the bedside. These experiences demonstrate a greater level of loneliness, difficulties in decision-making and communication, and an intense emotional impact on patients, their families, and clinicians.ĬOVID-19 has, unfortunately, created a heightened level of loneliness for hospitalized patients at end of life. The pandemic has impacted the end-of-life care experience of hospitalized patients and practitioners in profound ways. A notable unanticipated consequence of COVID-19 is the impact on palliative care practitioners treating COVID-19 and non-COVID-19 patients, especially in caring for patients at end of life. While adhering to mandatory physical distancing policies to prevent the spread of the virus, healthcare providers have been challenged to adapt to continuous changes in procedures while caring for patients. 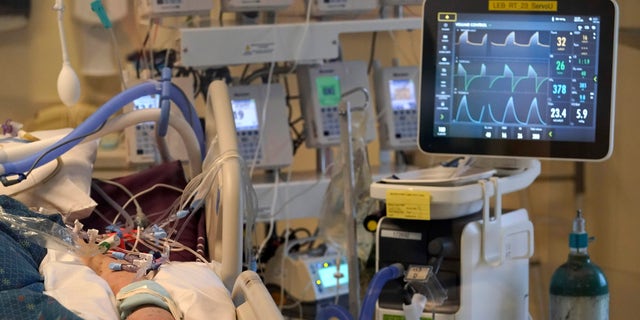
COVID-19 was officially declared a pandemic on March 11, 2020, altering healthcare practices in numerous ways. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
